Beyond Medication: Alternative Pain Management Options in 2026
Chronic pain affects millions of people, yet medication alone doesn’t always provide lasting relief—or the quality of life patients are looking for. In 2026, pain management is increasingly focused on a more comprehensive, personalized approach that goes beyond prescriptions.
From advanced therapies like Transcranial Magnetic Stimulation (TMS) to lifestyle-based strategies, today’s treatment landscape offers more options than ever to address both the physical and neurological components of pain.
Why Look Beyond Medication?
While medications can play an important role in pain control, they may not address the underlying causes of chronic pain. In some cases, patients also seek alternatives due to side effects, tolerance concerns, or a desire for more sustainable, long-term solutions.
Modern pain management focuses on:
- Reducing pain signals at the neurological level
- Supporting the body’s natural healing processes
- Improving function, mobility, and daily comfort
This shift has led to increased interest in non-invasive, drug-free therapies.
Understanding TMS for Pain Relief
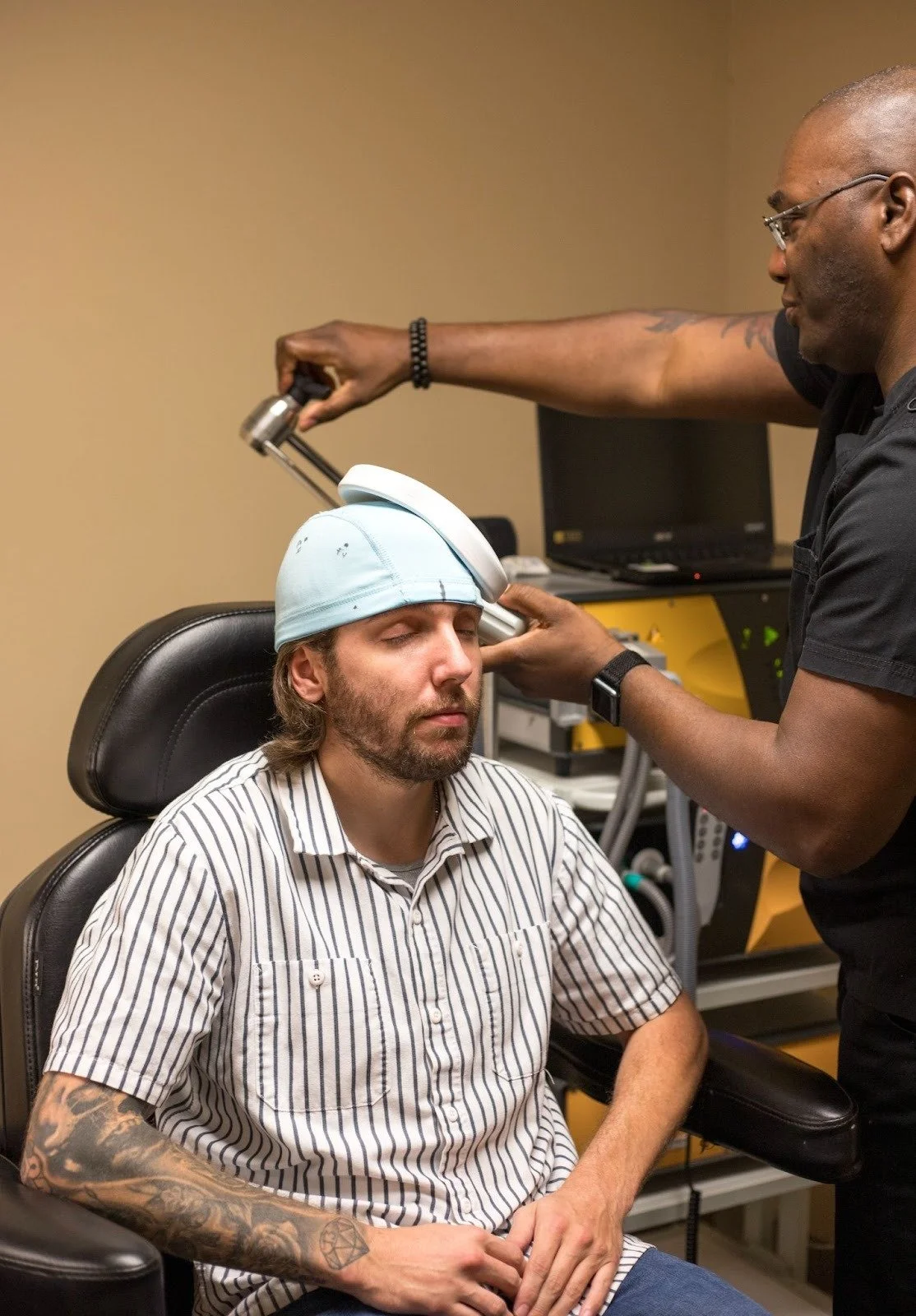
Transcranial Magnetic Stimulation is a non-invasive treatment that uses targeted magnetic pulses to stimulate specific areas of the brain involved in pain processing.
Originally developed for depression, TMS is now being explored and utilized as part of a broader approach to chronic pain management.
How TMS May Help with Pain
TMS works by modulating neural activity, which may:
- Alter how the brain perceives pain signals
- Reduce central sensitization (heightened pain response)
- Support improved regulation of mood and stress, which can influence pain perception
For some patients, this can translate into meaningful improvements in daily comfort and function over time.
TMS Side Effects and What to Expect
When considering TMS, many patients ask about potential side effects and overall comfort.
Common TMS Side Effects
TMS is generally well tolerated, but some patients may experience:
- Mild scalp sensitivity at the treatment site
- Temporary headache after sessions
- Light facial muscle twitching during treatment
These effects are typically short-lived and tend to improve as treatment continues.
TMS Discomfort: Is It Painful?
Patients often describe TMS discomfort as a tapping or pulsing sensation on the scalp. While it can feel unusual at first, most individuals adapt quickly within the first few sessions.
Settings can also be adjusted to improve comfort while maintaining therapeutic effectiveness.
A Realistic Timeline for Pain Reduction
One of the most important aspects of any alternative pain treatment is setting appropriate expectations.
With TMS and similar therapies, results are typically gradual rather than immediate.
General Timeline
- First 1–2 weeks: Adjustment period; mild symptom changes may begin
- Weeks 3–4: Many patients start noticing improvements in pain intensity or frequency
- Weeks 4–6+: Continued progress with more consistent relief for some individuals
It’s important to note that response varies based on the type of pain, duration of symptoms, and individual physiology.
Complementary Strategies for Long-Term Relief
TMS is often most effective when combined with other non-medication approaches. A comprehensive plan may include:
1. Movement and Physical Therapy
Targeted exercise can help restore mobility, reduce stiffness, and improve strength without overloading sensitive areas.
2. Stress and Nervous System Regulation
Chronic pain is closely tied to the nervous system. Techniques such as:
- Mindfulness
- Breathwork
- Biofeedback
can help reduce pain amplification linked to stress.
3. Sleep Optimization
Poor sleep can worsen pain sensitivity. Improving sleep quality may support better recovery and overall pain control.
4. Nutritional Support
Anti-inflammatory nutrition and hydration can play a role in how the body processes pain and heals.
The Future of Pain Management
In 2026, the most effective pain management strategies are no longer one-dimensional. Instead, they combine innovative therapies like TMS with personalized lifestyle and wellness approaches.
This shift reflects a growing understanding that pain is not just physical—it is neurological, emotional, and behavioral as well.
When to Consider Alternative Pain Treatments
You may benefit from exploring options beyond medication if:
- Pain persists despite standard treatments
- Medication side effects are difficult to manage
- You are seeking a more comprehensive, non-invasive approach
- Your pain is influenced by stress, mood, or neurological factors
A personalized consultation can help determine whether TMS or other therapies may be appropriate for your needs.
Final Thoughts
Alternative pain management is not about replacing medication entirely—it’s about expanding your options. Treatments like Transcranial Magnetic Stimulation offer a different pathway by addressing how the brain processes pain, rather than only targeting symptoms.
With the right combination of therapies, many patients are able to achieve meaningful improvements in comfort, function, and overall quality of life.
If you’re exploring alternatives to medication for chronic pain, a personalized evaluation can help determine whether TMS or other non-invasive therapies may be appropriate for you. Contact Mind + Body Medicine in Dallas to schedule a consultation and learn more about your options for long-term pain management.